Shots were fired. The Senate was supposedly under siege. Some senators were live streaming from within – and you could tell that it was really staged. Bad acting. Seriously, if you’re being assassinated or the senate was under attack, why wait until all the minority senators were not present any longer? Why the chill moments with DILG secretary Jonvic Remulla strutting in and striking a post with the remaining senators? Wouldn’t they all have been more terrified like the reporters were? The situation didn’t seem that natural because the crowd were all too scared while the senators and the full battle geared up security guards of the OSAA were, for the lack of a better description, relaxed.
With the facts all in from the Wednesday chaos, we now know more verified information.
- Mao Aplasca replaced Ret Maj Gen Rene Samonte, who was OSAA chief, after a scathing confrontation when Bato de la Rosa suddenly appeared and reprimanded (bullied should be the more appropriate term) Samonte for allowing the NBI agents into the Senate complex last May 11.
- Samonte resigned right there and then after the verbal abuse of Bato. Prompting Bato to nominate Aplasca (a former military academy classmate) to take his place. Because Alan Peter had already taken the helm as Senate President, the resolution was approved immediately.
- There was obviously more tension building up between the now minority and the majority force. Robinhood Padilla became interruptive during sessions when Kiko Pangilinan was still speaking prompting reactions from both camp sides. Of course, as all thugs would go, the actor did not take it well.
- That show of force had led to the setting where the disarray of May 13 would come into play. Shots were fired and as the video of the news reporters were being pieced together and as reports were coming in based on actual timeline – the NBI was NOT in the senate building but in the GSIS part of the GSIS building. If people don’t know, the senate is RENTING only from the GSIS space (that’s why they’re building a senate building in Taguig which is now amounting to a billions of pesos over priced). This is in contrast to what Aplasca was saying. His claim is that the NBI was in the senate building and that he had fired a warning shot when he saw they were armed. This was in stark contrast to videos showing that shots had been fired in the senate building and the NBI were in the GSIS building and had rushed to where the shots were being fired. Imagine that!!! 27-30 bullets were supposedly warning shots…now how stupid is that?
- The OSAA is security detail for the senate. They are not law enforcement officers. They are security guards. That includes Aplasca who was once a General but has been retired since 2019 from the Philippine National Police. He forgets that he is NOT a police officer any longer. That engagement between the OSAA and the NBI, was a tail of fiction.
- During the live interviews with Bato, he was babbling like a frightened criminal, seeking shelter from his comrades. His sudden appearance after 6 months in hiding was the clincher. Someone was up to something and they had a plan. This was the plan.
The investigations during the chaos clearly show that the events leading up to the ‘escape’ and press conference of Alan Peter was obviously a diversionary tactic. If Bato was free to come and go because he is not under arrest but only protective custody, then why all the drama? He could have just left in a car at 6pm or the day before when there was a standoff.

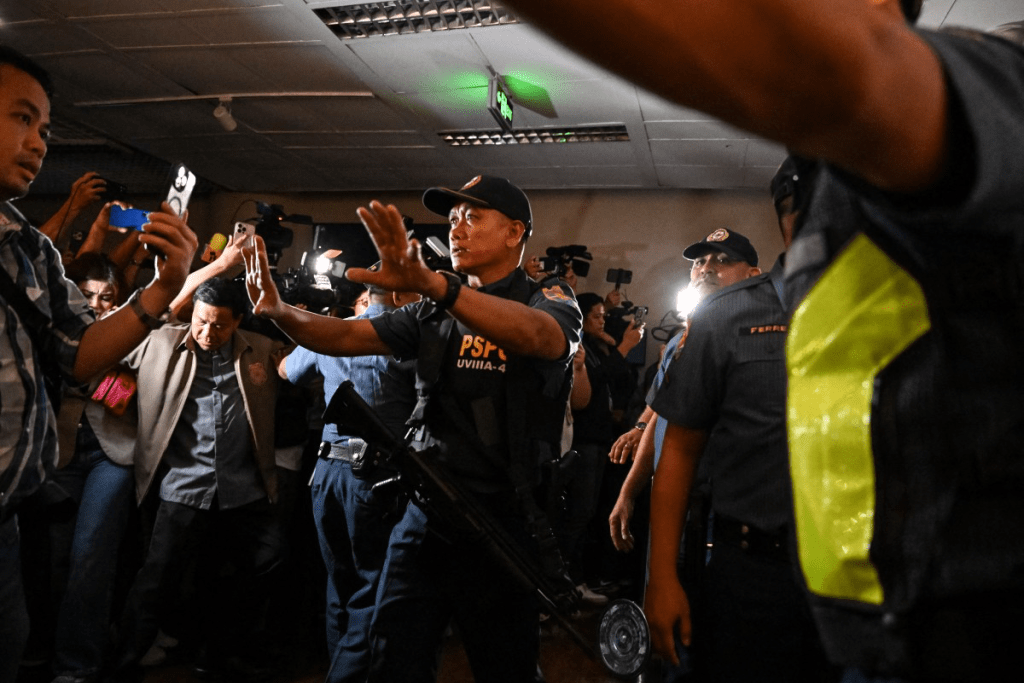
It was a poorly written script that would fire back at them, just to have Bato come and go.
The disruption in the Senate is not acceptable.
The behavior of the Senators including that of Imee Marcos is deplorable.
Those who connived in this grand scheme should be held accountable.
Because the reputation of that Senate has been tarnished forever.
And no matter how things go with the transmittal of the impeachment complaint versus Sara Duterte and the eventual judicial process in the senate when the sit en banc as judge and jury – all eyes of the Filipino people will be on every senator and they will hold them ALL accountable for justice or injustice at the end of the day.
[Photos from CDN Digital https://www.facebook.com/photo?fbid=1407454624747878&set=pcb.1407315408095133]